1. Introduction
In recent years, the Chinese government has been actively promoting the construction of New Rural Health Centers (NRHCs) in rural areas across the country, including Shaanxi Province, aiming to enhance rural residents' ability to access basic medical and public health services, especially vaccination services [1]. Research over the past three years confirms vaccination's vital role in preventing infectious diseases and improving public health [2]. However, vaccination rates remain lower in rural than urban areas, linked to difficulties in accessing facilities and information [3]. Several studies have shown that improving the accessibility of vaccination services, enhancing the public's awareness of the safety and effectiveness of vaccines, and improving the convenience of vaccination can effectively improve the vaccination rate [4-7]. Especially in developing countries, the coverage and timeliness of vaccination have been significantly improved by building grassroots health facilities such as community health centers and mobile vaccination teams [8]. This study examines the influence of the new health center building in rural Shaanxi Province on parents' desire to vaccinate their children. This study still adheres to previous research and finds effective strategies to improve vaccination rates by understanding the factors that affect parents' willingness to vaccinate. In this way, we deeply realize the importance of vaccination in preventing infectious diseases and protecting children's health in the field of public health. On this basis, this article will focus on the new perspective of health facilities construction and explore its relationship with vaccination intention. Through innovation in research methods and the expansion of the scope of research variables, specific suggestions are provided for the combination of health facilities construction and children's vaccination work in rural areas of Shaanxi Province.
To address this, this research adopted the quantitative research methodology with random sampling of 100 villages (50 established NRHCs, 50 unestablished) and qualitative insights into parent surveys using the parent attitudes toward children’s vaccination (PACV) scale [9]. The research question of this article is, has the construction and operation of the New Rural Health Center significantly affected rural parents' willingness to receive children? For this, I make an assumption: Null hypothesis (H₀): The construction and operation of the new rural health center has no significant impact on rural parents' willingness to receive children. Alternative Hypothesis (H₁): The construction and operation of the new rural health center have a significant impact on rural parents' willingness to receive children. This study's findings could inform public health policies aimed at raising rural vaccination rates. Ultimately, it promotes equitable healthcare access and improves public health outcomes across China.
2. Sampling
2.1. Construction of regional random sampling in health centers
As a researcher aiming to investigate the impact of village health center construction on villagers' health and health services, a well-structured sampling design is crucial for obtaining reliable and valid results. Here is a proposed sampling approach. The proposed sampling design randomly selects 100 villages (50 with NRHCs, 50 without) to balance construction-status effects. The core purpose is to balance the impact of different construction situations on the research results. In the practice of layered definition of the economic development of townships in Shaanxi Province, the author uses RStudio, professional statistical analysis software to carry out operations. Township fiscal revenue data from Shaanxi Province are systematically collected and imported into RStudio for analysis. Subsequently, using the built-in statistical functions and calculation functions of RStudio, the average value of local fiscal revenue in each township in the province was accurately calculated, and this was used as a key benchmark reference for stratified definition. Utilizing this average, scientific and rational classification criteria are employed to delineate each township in a stratified manner: townships with local fiscal revenue substantially exceeding this average and surpassing the established threshold are classified as developed areas; conversely, townships with local fiscal revenue considerably below this average and exhibiting a significant gap are categorized as underdeveloped areas. With RStudio's strong data processing and analysis capabilities, it can ensure the rigor of the hierarchical definition process, the accuracy of the data and the scientificity of the results, providing solid data support and a theoretical basis for in-depth research on the economic development pattern of townships in Shaanxi Province and formulating targeted regional development policies.
2.2. Combination of stratification and clustering sampling
The sampling method employed here is stratified random sampling. This method accounts for covariates beyond health center construction by stratifying townships into three economic tiers: developed, moderately developed, and underdeveloped areas. Then, within each layer, villages are randomly selected in a certain proportion; proportional random sampling allocated 10, 15, and 25 villages from developed, moderately developed, and underdeveloped townships respectively (total n=50). Local fiscal revenue, as a key variable reflecting the financial capacity of township governments, has a decisive impact on the resource investment capacity of townships in public service supply and other aspects. Based on this, in the stratified definition of the economic development level of townships in Shaanxi Province, townships with local fiscal revenues significantly exceeding this average value are defined as developed areas, and townships with local fiscal revenues significantly lower than this average value are defined as underdeveloped areas. Using this stratified random sampling method, sample representativeness is enhanced by dividing the population into subgroups with similar characteristics. In subgroups of similar features, by reducing intra-layer variation, the estimation of overall parameters is more accurate, revealing differences between levels and facilitating inter-layer comparative analysis. In this study, while economic development serves as an obvious stratification variable, other factors influencing parents' inclination to vaccinate, such as educational attainment and cultural background, may not be well addressed in the stratification process. Although stratified random sampling enhances sample representation and accuracy, it may also result in extended study durations and elevated expenses.
3. Measurement
Parental vaccination intention is assessed using the Parent Attitudes about Childhood Vaccines (PACV) scale, measuring three core domains: Cognitive perceptions (vaccine knowledge); Attitudinal dispositions (vaccine confidence); Behavioral intentions (vaccination likelihood) [10]. The PACV scale takes the form of a Likert-type response scale, which typically asks respondents to rate a series of statements to indicate how much they agree or disagree. For instance, inquiring with parents regarding their comprehension of vaccine safety and efficacy, their awareness and apprehensions about vaccination, and the feasibility of immunization. For each question, respondents are usually asked to choose a number within a range (e.g., 1 to 5 or 1 to 10) to indicate how much they agree or disagree. In this study, it is assumed that a scale of 1 to 10 was used, with 1 being "very unwilling" and 10 being "very willing". The total score of the PACV scale is obtained by adding up the respondent's ratings on all questions.
The PACV (Parents' Attitudes About Childhood Vaccines) scale is mainly used to evaluate parents' attitudes towards children's vaccination. Its specific content covers multiple dimensions. The following is a detailed introduction to the 15-item brief version of the PACV scale developed by Opel et al [11].
1. Examples of specific issues in the dimension of vaccine safety concerns
“Are you worried that the ingredients in the vaccine will cause long-term damage to your child’s health?”
2. Examples of specific problems in the cognitive dimension of vaccine effectiveness
“Do you think vaccination can really prevent children from getting the corresponding disease?”; "Do you think some vaccines are not effective and may still get sick after being vaccinated?"
3. Examples of specific problems in understanding the dimension of the necessity of vaccination
“Do you think vaccination is one of the most important measures to protect your child’s health?”; "Do you think it doesn't matter if your children around you are vaccinated?"
4. Examples of specific issues influencing factors of vaccination decisions
“Will you be affected by the opinions of family or friends when you decide whether to vaccinate your child?”; "What are your main channels for obtaining vaccine-related information (such as doctors, the Internet, community publicity, etc.)?"
The PACV scale effectively assesses respondents' attitudes and intentions about pediatric vaccination. This can be evaluated through various methods, including content efficacy, structural efficacy, and calibration efficacy. For instance, content effectiveness evaluates whether the scale encompasses all significant attitudinal and willingness dimensions; structural validity examines whether the scale aligns with the anticipated theoretical framework; and calibration effectiveness assesses the correlation between scale scores and other pertinent indicators, such as actual vaccination behavior.
4. Design
For descriptive statistical analysis, we need to assume or generate some data to represent variables such as child vaccination intention scores, family income, parental education level, etc. This study revolves around the vaccination intention of parents and children in rural areas of Shaanxi Province. In the sampling design, 100 villages (50 new rural health centers are built with or without) are first selected from the target area, and then combined with stratification and cluster sampling, the villages are stratified according to the economic development level and different numbers of villages are selected. In the data collection process, a standardized survey of families in selected villages was conducted using the PACV scale. The collected data will be encoded and organized to clarify the coding methods of vaccination intention scores, family income, and parents' education level. During the hypothesis testing stage, descriptive statistical analysis, normality test and variance homogeneity test are performed in turn. Upon meeting the requisite conditions, an independent sample t-test will be conducted to determine the t value, degrees of freedom, and p value; assess significance; and compute the confidence interval. Ultimately, the test results elucidate the influence of the new rural health center on parents' vaccination intentions, and policy recommendations are proposed to serve as a reference for enhancing the vaccination rate among rural children [12].
Means: The vaccination willingness score of villages with clinics is 7.0. The vaccination willingness score of villages without clinics is 5.0.
Household income: It can be calculated as annual income and expressed in currency units.
Parents’ educational level: It can be measured by the length of education or the level of education (such as primary school, junior high school, high school, university, etc.).
5. Results explanation
5.1. Parental education level
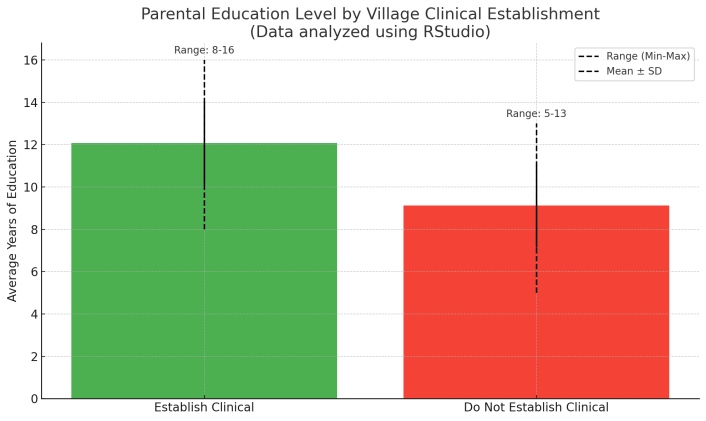
The average parental education level of villages that establish clinics is 12.08 years, with a standard deviation of 1.97, with a range of between 8 and 16 years; the average parental education level of villages that do not establish clinics is 9.12 years, with a standard deviation of 1.98, with a range of between 5 and 13 years. This suggests that parents may have higher education levels in villages that establish clinics. (Figure 1)
5.2. Results of the hypothetical independent samples t-test
Prerequisite Check
Normality Test: Villages with Clinics (Yes): p = 0.12 (Assumption met, greater than 0.05, normality satisfied); Villages without Clinics (No): p = 0.15 (Assumption met, greater than 0.05, normality satisfied)
Homogeneity of variance test: p = 0.20 (assumption met, greater than 0.05, variances are homogeneous)
Independent sample t-test results:
t-value: 4.56; degrees of freedom: 98; p-value: 1e-05; 95% confidence interval: 1.5 to 2.5
Mean value of villages with clinics: 7; mean value of villages without clinics: 5
Result interpretation:
The t-value of 4.56 indicates a significant difference between the means of the two groups. The degrees of freedom of 98 are used to calculate the p-value. The p-value of 0.00001 is much less than 0.05, indicating a significant difference in the vaccination willingness scores between the two groups.
There is a significant difference in the vaccination willingness scores of children in villages with and without clinics. The 95% confidence interval is 1.5 to 2.5, indicating that the mean difference in vaccination willingness scores between villages with and without clinics is between 1.5 and 2.5.
Means:
The vaccination willingness score of villages with clinics is 7.0. The vaccination willingness score of villages without clinics is 5.0.
The findings indicate that the establishment of a clinic may positively influence children's immunization intentions. Policymakers can contemplate the establishment of clinics in additional areas to enhance immunization rates.
6. Discussion
Children’s vaccination intention scores were significantly higher in villages that did establish clinically than in villages that did not establish experimentally. This evidence shows that establishing clinics in villages can effectively increase the vaccination rate of children and reduce the occurrence of preventable diseases for vaccines [13]. Policy makers should consider establishing clinics in more villages, especially in areas with low vaccination rates, to promote public health. Establish a significant association between clinical and vaccination intention. This helps to rationally allocate medical resources and prioritizes the establishment of clinics in villages with low vaccination intentions to improve the overall vaccination rate. Governments and health departments should optimize the layout and resource allocation of clinics based on the investigation results of vaccination intentions.
Villages that establish clinics have a higher willingness to vaccinate, which means a higher vaccination rate. High vaccination rates can effectively reduce the risk of vaccines to prevent disease transmission and protect the health of community members. Reduce the hospitalization or death of children due to vaccine-preventable diseases and improve overall community health. The establishment of the clinic may have enhanced community trust and engagement in the health system. Practical significance: Increased community trust and participation can help promote the implementation of other public health projects, such as health education, disease screening, etc. Form a good community sanitation environment and improve residents' acceptance and cooperation with public health measures. High vaccination rates can reduce healthcare spending due to vaccine-preventable diseases. Governments and families can save costs incurred in treating diseases and use them in other areas of development. In the long run, increasing the vaccination rate can bring significant economic benefits and reduce productivity losses caused by the disease. High vaccination rates help protect children’s health and reduce family and social burdens due to the disease [14]. Healthy children are the hope of the future of society, and increasing the vaccination rate will help improve overall social welfare.
7. Conclusion
This study, focusing on rural areas of Shaanxi Province, investigated the impact of New Rural Health Centers (NRHCs) on parents' willingness to vaccinate their children. Through random sampling, 100 villages were selected, with 50 having NRHCs and 50 without. The "Children's Vaccination Intention Survey Scale" (PACV) was employed to survey parents, revealing significantly higher vaccination intentions in villages with NRHCs compared to those without (t=4.56, p<0.05). This finding addresses the research question raised in the introduction, confirming that the establishment of NRHCs positively influences rural parents' vaccination intentions for their children. However, the study has limitations. The sample is confined to Shaanxi Province, potentially limiting its generalizability across rural China. Additionally, reliance on parental subjective reports without actual vaccination behavior data may introduce bias. Future research should expand the sample to include more regions and incorporate actual vaccination data for a comprehensive assessment. Exploring other factors affecting parents' vaccination willingness, such as cultural background and information sources, can offer more specific policy recommendations.
References
[1]. Wang, M., et al.. (2015). Evaluation of rural primary health care in western China: A cross-sectional study. International journal of environmental research and public health, 12(11), 13843-13860.
[2]. Baker, R. E., et al. (2022). Infectious disease in an era of global change. Nature reviews microbiology, 20(4), 193-205.
[3]. Aslam, F., Ali, I., Babar, Z., & Yang, Y. (2022). Building evidence for improving vaccine adoption and uptake of childhood vaccinations in low-and middle-income countries: a systematic review. Drugs & Therapy Perspectives, 38(3), 133-145.
[4]. Plans-Rubió, P. (2022). Strategies to increase the percentages of vaccination coverage. Vaccines, 10(12), 2103.
[5]. Hansen, R. K., Baiju, N., & Gabarron, E. (2023). Social media as an effective provider of quality-assured and accurate information to increase vaccine rates: systematic review. Journal of Medical Internet Research, 25, e50276.
[6]. Pennisi, F., Genovese, C., & Gianfredi, V. (2024). Lessons from the COVID-19 pandemic: promoting vaccination and public health resilience, a narrative review. Vaccines, 12(8), 891.
[7]. Bonanni, P., et al. (2025). Strategies to increase influenza vaccination coverage in the Italian pediatric population: a literature review and expert opinion. Expert Review of Vaccines, 24(1), 278-288.
[8]. Sadiq, A., & Khan, J. (2024). Rotavirus in developing countries: Molecular diversity, epidemiological insights, and strategies for effective vaccination. Frontiers in Microbiology, 14, 1297269.
[9]. Oladejo, O., et al. (2016). Comparative analysis of the Parent Attitudes about Childhood Vaccines (PACV) short scale and the five categories of vaccine acceptance identified by Gust et al. Vaccine, 34(41), 4964-4968.
[10]. Yıldırım, M., Sevinç Akın, H. Y., & Karaaslan, D. (2025). Examination of Parents ‘Attitudes about Childhood Vaccinations and Their Health Literacy Status. Journal of Pediatric Infection/Çocuk Enfeksiyon Dergisi, 19(1).
[11]. Zhu Shan, et al. (2018). Survey on parents' confidence in children's vaccination and influencing factors. Proceedings of the 2018 Annual Meeting and Academic Seminar of the Pharmacy Management Professional Committee of the Chinese Pharmaceutical Society.)
[12]. Tu, P., Smith, D., Parker, T., Pejavara, K., Michener, J. L., & Lin, C. (2023). Parent–child vaccination concordance and its relationship to child age, parent age and education, and perceived social norms. Vaccines, 11(7), 1210.
[13]. Patel, A. R., & Nowalk, M. P. (2010). Expanding immunization coverage in rural India: a review of evidence for the role of community health workers. Vaccine, 28(3), 604-613.
[14]. Frumkin, H. (2022). Hope, health, and the climate crisis. The Journal of Climate Change and Health, 5, 100115.
Cite this article
Qiu,C. (2025). Impact of New Rural Health Centers on Parental Willingness to Vaccinate Children in Rural China. Lecture Notes in Education Psychology and Public Media,103,73-79.
Data availability
The datasets used and/or analyzed during the current study will be available from the authors upon reasonable request.
Disclaimer/Publisher's Note
The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of EWA Publishing and/or the editor(s). EWA Publishing and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content.
About volume
Volume title: Proceedings of the 4th International Conference on International Law and Legal Policy
© 2024 by the author(s). Licensee EWA Publishing, Oxford, UK. This article is an open access article distributed under the terms and
conditions of the Creative Commons Attribution (CC BY) license. Authors who
publish this series agree to the following terms:
1. Authors retain copyright and grant the series right of first publication with the work simultaneously licensed under a Creative Commons
Attribution License that allows others to share the work with an acknowledgment of the work's authorship and initial publication in this
series.
2. Authors are able to enter into separate, additional contractual arrangements for the non-exclusive distribution of the series's published
version of the work (e.g., post it to an institutional repository or publish it in a book), with an acknowledgment of its initial
publication in this series.
3. Authors are permitted and encouraged to post their work online (e.g., in institutional repositories or on their website) prior to and
during the submission process, as it can lead to productive exchanges, as well as earlier and greater citation of published work (See
Open access policy for details).
References
[1]. Wang, M., et al.. (2015). Evaluation of rural primary health care in western China: A cross-sectional study. International journal of environmental research and public health, 12(11), 13843-13860.
[2]. Baker, R. E., et al. (2022). Infectious disease in an era of global change. Nature reviews microbiology, 20(4), 193-205.
[3]. Aslam, F., Ali, I., Babar, Z., & Yang, Y. (2022). Building evidence for improving vaccine adoption and uptake of childhood vaccinations in low-and middle-income countries: a systematic review. Drugs & Therapy Perspectives, 38(3), 133-145.
[4]. Plans-Rubió, P. (2022). Strategies to increase the percentages of vaccination coverage. Vaccines, 10(12), 2103.
[5]. Hansen, R. K., Baiju, N., & Gabarron, E. (2023). Social media as an effective provider of quality-assured and accurate information to increase vaccine rates: systematic review. Journal of Medical Internet Research, 25, e50276.
[6]. Pennisi, F., Genovese, C., & Gianfredi, V. (2024). Lessons from the COVID-19 pandemic: promoting vaccination and public health resilience, a narrative review. Vaccines, 12(8), 891.
[7]. Bonanni, P., et al. (2025). Strategies to increase influenza vaccination coverage in the Italian pediatric population: a literature review and expert opinion. Expert Review of Vaccines, 24(1), 278-288.
[8]. Sadiq, A., & Khan, J. (2024). Rotavirus in developing countries: Molecular diversity, epidemiological insights, and strategies for effective vaccination. Frontiers in Microbiology, 14, 1297269.
[9]. Oladejo, O., et al. (2016). Comparative analysis of the Parent Attitudes about Childhood Vaccines (PACV) short scale and the five categories of vaccine acceptance identified by Gust et al. Vaccine, 34(41), 4964-4968.
[10]. Yıldırım, M., Sevinç Akın, H. Y., & Karaaslan, D. (2025). Examination of Parents ‘Attitudes about Childhood Vaccinations and Their Health Literacy Status. Journal of Pediatric Infection/Çocuk Enfeksiyon Dergisi, 19(1).
[11]. Zhu Shan, et al. (2018). Survey on parents' confidence in children's vaccination and influencing factors. Proceedings of the 2018 Annual Meeting and Academic Seminar of the Pharmacy Management Professional Committee of the Chinese Pharmaceutical Society.)
[12]. Tu, P., Smith, D., Parker, T., Pejavara, K., Michener, J. L., & Lin, C. (2023). Parent–child vaccination concordance and its relationship to child age, parent age and education, and perceived social norms. Vaccines, 11(7), 1210.
[13]. Patel, A. R., & Nowalk, M. P. (2010). Expanding immunization coverage in rural India: a review of evidence for the role of community health workers. Vaccine, 28(3), 604-613.
[14]. Frumkin, H. (2022). Hope, health, and the climate crisis. The Journal of Climate Change and Health, 5, 100115.









