1. Introduction
The health risks of smoking have long been widely recognized, with lung cancer being one of its most serious and deadly diseases. According to the World Health Organization, about 85 per cent of lung cancer cases worldwide can be directly attributed to tobacco use [1]. Despite extensive public health promotion and tobacco control campaigns in recent years, smoking prevalence has not decreased significantly in many countries, especially in low- and middle-income countries.
Several previous studies have focused on the correlation between smoking prevalence and lung cancer mortality. For example, Smith et al. conducted a longitudinal analysis across over 50 countries and found that the higher smoking prevalence is consistently associated with higher lung cancer mortality rate [2]. In addition, Johnson noted that even a slight decrease in smoking prevalence resulted in a significant reduction in lung cancer incidence [3]. These studies emphasize the importance of sustained control of smoking behavior in reducing the disease burden of lung cancer.
This paper uses a literature review to analyze the causal relationship between smoking prevalence and lung cancer incidence in different countries, with the aim of providing policy recommendations and theoretical support for global public health. The significance of the study is not only to deepen people's knowledge of the risks of smoking, but also to provide a scientific basis for the development of effective tobacco control strategies.
2. Biological mechanisms of lung cancer caused by tobacco smoking
Tobacco smoke contains more than 7,000 chemical constituents, of which at least 70 have been recognized as carcinogens, including polycyclic aromatic hydrocarbons (PAHs), tobacco-specific nitrosamines (TSNAs), benzene, arsenic, cadmium and formaldehyde. These substances can directly damage the DNA of lung epithelial cells in ways that include the formation of DNA adducts or the induction of reactive oxygen species (ROS) production, which can lead to genomic instability and the development of mutations [4]. For example, PAHs are metabolically activated in the lungs to form bulky adducts that interfere with DNA replication, while TSNAs alkylate bases, triggering point mutations and chromosomal abnormalities.
In addition to directly inducing mutations, tobacco smoke impairs the body's DNA repair system, including nucleotide excision repair and base excision repair pathways, making cells less capable of repairing mutations and mutations more likely to accumulate. Meanwhile, long-term exposure to tobacco smoke can also lead to epigenetic alterations, such as hypermethylation of promoter regions of oncogenes (e.g., p53, CDKN2A), which can inhibit their expression and cause cells to lose normal regulation of division and apoptosis [1, 4].
Chronic smoking leads to clonal expansion of mutant cells, especially in genes controlling cell proliferation, DNA repair and apoptosis. Genome-wide studies have shown that smokers carry a significantly higher number of mutations in lung cancer tumors than non-smokers, and the key genes mutated include oncogenes (e.g., KRAS, EGFR) and oncogenes (e.g., TP53) [1]. These molecular impairments provide the basis for the development of lung cancer and usually manifest as disease many years after first smoking.
Epidemiologic data rovides compelling support for the link between smoking and lung cancer. Smokers face a elevated dramatically risk of developing lung cancer, ranging from 15 to 30 times higher than that of nonsmokers. This risk rises with increasing years and intensity of smoking. Notably, despite a gradual decrease in lung cancer risk after smoking cessation, ex-smokers still retain a higher risk compared to those who have never smoked. This persistent risk is attributed to the irreversible genetic and epigenetic alterations induced by prior smoking exposure [1].
3. Global trends and regional variations
3.1. Global smoking and lung cancer trends
Globally, there is a significant positive correlation between smoking prevalence and lung cancer mortality. For example, according to Our World in Data, China has a smoking prevalence of 25.6% and a lung cancer mortality rate of 34.8 per 100,000 people, whereas Australia has a smoking prevalence of only 13.6% and its lung cancer mortality rate is significantly lower [5-6]. This difference suggests that national-level tobacco control policies play a key role in regulating smoking behavior and reducing cancer burden.
The analysis shown in Figure 1 and Figure 2 further validates this trend: countries with higher smoking prevalence tend to be accompanied by higher lung cancer incidence. Despite differences in socioeconomic status, healthcare resources, and cultural practices across countries, the association between smoking and cancer showed a high degree of consistency across countries of different income levels. Particularly in low- and middle-income countries, limited capacity for tobacco control enforcement has contributed to high and even rising smoking prevalence, which has exacerbated public health challenges.
To complement the observations at the global level, this study further conducted multiple linear regression analyses using individual data to examine the effects of age and smoking history on cancer risk. The results show that both age and smoking status (especially “ex-smokers”) were highly significant predictors of cancer occurrence (p < 2e-16). The regression coefficient for the age variable was 0.00367, indicating that the risk of cancer increases steadily with age, while the coefficient for ex-smokers was -0.02293, indicating that the risk was significantly higher than that of never-smokers, although the risk was reduced after quitting smoking. This statistical model provides micro-level support and further corroborates the findings of the global data that smoking history remains an important independent risk factor for cancer development, even after controlling for other demographic variables.
To further visualize the combined effect of age and smoking history on cancer risk, Figure 1 illustrates the cancer incidence rates of current and former smokers in different age groups. It is clear from the figure that cancer risk increases with age, with current smokers consistently having higher cancer incidence rates than ex-smokers in all age groups.
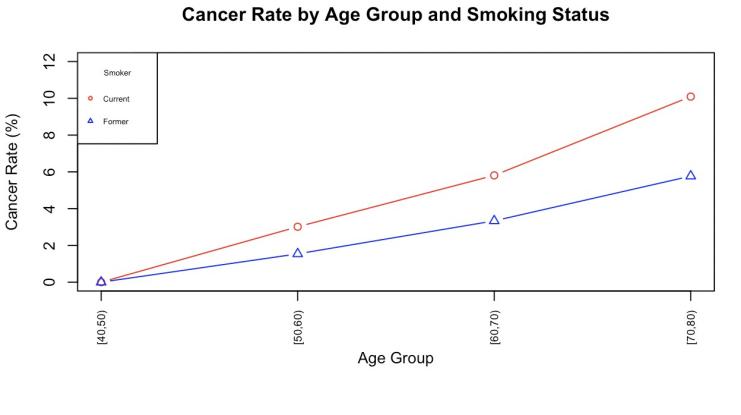
This trend is consistent with the results of the previous regression analyses, suggesting that although smoking cessation reduces the risk of cancer, the long-term biological damage it causes remains. The persistent incidence gap between current and former smokers further emphasizes the importance of “quitting early” in reducing cumulative risk.
3.2. Regional variations analysis
Results of linear regression, with race and smoking status as independent variables, revealed that “smokerFormer” was the only statistically significant variable (p < 2e-16). The regression coefficient for “smokerFormer” was -0.01857, implying that ex-smokers had a significant reduction in cancer risk of approximately 1.86% compared to current smokers. While the regression coefficients for race variables such as Asian, African-American, and White differed, their p values were all greater than 0.05, which was statistically insignificant, suggesting that there is not much difference in cancer risk between races while controlling for smoking behavior. This result further validates that: Smoking behavior itself is the main factor contributing to the elevated cancer risk, rather than racial differences. The coefficient of determination, R², of the model was 0.0025, indicating that cancer risk is also influenced by a variety of other factors, but the independent effect of smoking remains significant.
Although Figure 2 illustrates the distribution of cancer incidence rates based on race, gender, and smoking status rather than by country, trends that characterize some countries can be inferred from it. For example, the United States has the highest cancer incidence rates among current smokers in American Indian or Alaska Native populations, reflecting their persistent health disparities in access to tobacco control interventions and cessation resources. Asian populations (e.g., China, Japan, and South Korea) have lower overall cancer incidence rates, particularly among ex-smokers, which may be related to their greater genetic detoxification capacity or cultural habits of discontinuing smoking earlier. Differences in incidence rates between current and ex-smokers in the white population, which is widely distributed in North America, Europe, and Australia, are significant, reflecting the effectiveness of tobacco control policies. Cancer risk was higher among current smokers but decreased among ex-smokers among African Americans, which may be influenced by structural differences in cessation support and access to health care resources. Overall, the racial patterns in Figure 2 reflect, in part, the effectiveness of tobacco control policy implementation, socioeconomic disparities, and access to public health systems across countries.
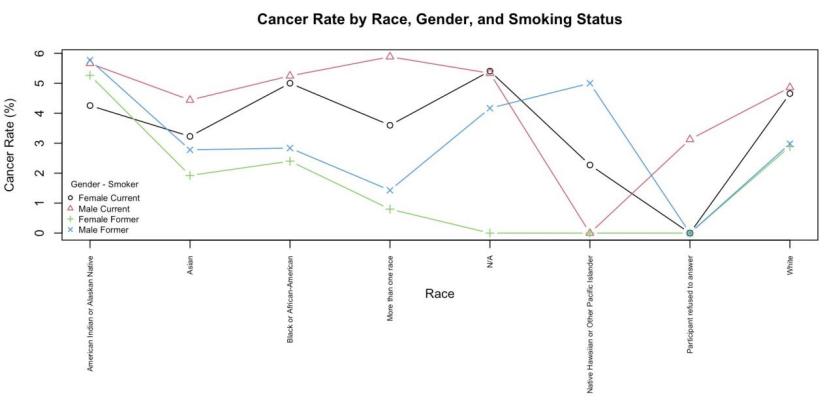
4. Influence of socioeconomic factors on smoking behavior
Socioeconomic status (SES) significantly influences an individual's smoking behavior [7]. Individuals with low SES often experience higher levels of life stress, lower health literacy, and limited access to health information. Additionally, they are more likely to be exposed to cheaper, yet more harmful, tobacco products [8]. Two key factors are education level and income level. Those with higher education levels are usually more aware of the long-term health risks associated with tobacco. They are also more likely to accept advice on smoking cessation in public health campaigns, resulting in a stronger sense of health awareness and self-control [7]. In contrast, those with lower education levels may lack scientific knowledge of the dangers of tobacco, and even in cultural or social settings develop a sense of identification with smoking, increasing the risk of addiction.
Income level is also a determining factor. Lower-income individuals are more price-sensitive and tend to gravitate towards cheaper tobacco products, which often lack regulation or are of poorer quality [8]. In addition, tobacco companies also tend to focus their marketing on low-income communities, making them easier targets for consumption. In low-income countries such as Indonesia and Egypt, weak tobacco control regulations and the low price of tobacco have led to persistently high smoking rates, especially among the poor.
In contrast, high-income countries such as the United States and the United Kingdom have significantly reduced smoking prevalence through increased investment in education and the implementation of tobacco control policies (e.g., higher tobacco taxes, restrictions on advertising, health education, etc.) [1, 9]. In these countries, the public not only receives anti-tobacco education earlier, but also has better access to healthcare and cessation services [9]. These differences suggest that tobacco control strategies must be tailored to the local socioeconomic context, particularly in terms of education, income support, and access to health services, in order to develop effective and equitable interventions [7].
5. Practice and effectiveness of tobacco control policies
There is a large body of evidence that comprehensive tobacco control policies have achieved significant results globally. These policies typically include raising tobacco taxes, banning smoking in public places, installing health warning labels, and conducting anti-tobacco awareness campaigns [9]. According to the MPOWER framework proposed by the World Health Organization, countries that have fully implemented three or more tobacco control measures have the most significant downward trend in smoking prevalence.
For example, Australia is widely recognized as a global leader in tobacco control efforts. Through the early introduction of plain packaging for cigarettes, high tobacco taxes, and strong public health campaigns, Australia's adult smoking prevalence has fallen to less than 12%, with a corresponding decline in lung cancer mortality [10]. This case demonstrates the dramatic effects of multiple tobacco control measures implemented in concert and sustained.
In contrast, Indonesia presents a different picture. Despite having one of the highest male smoking prevalence rates in the world, tobacco control policies are relatively weak. Tobacco advertising is still prevalent, cigarette prices are low, and the ban on smoking in public places is poorly enforced. As a result, smoking prevalence continues to be high and tobacco-related diseases remain a serious public health burden [8].
China is a representative “intermediate” case. China has made considerable strides in recent years to outlaw smoking in public locations and add warning labels to cigarettes, but urban and rural areas execute policies quite differently. While smoking prevalence has declined in some major cities, it remains high in rural areas where regulation is weak and cultural attitudes are influential [5].
These country cases show that comprehensive tobacco control strategies are effective in reducing smoking prevalence and related diseases, but also face many challenges in implementation, especially in resource-limited areas. Therefore, sustained political commitment, public health education, and international collaboration are needed to achieve sustainable tobacco control efforts [9].
6. Conclusion
In summary, this paper systematically reviewed the causal relationship between smoking and lung cancer from four aspects: biological mechanisms, global trends, socioeconomic factors and policy responses. The findings suggest that smoking is still the most important cause of lung cancer and that effective tobacco control policies are a key means to reduce the incidence of lung cancer. The effectiveness of tobacco control policies varies from country to country, but successful experiences show that the combination of policy interventions and health education can effectively reduce smoking behaviors and thus reduce lung cancer incidence and mortality.
However, there are some limitations in this paper, mainly due to the fact that the data relied on secondary literature and failed to incorporate field research or original data modeling. Future studies could further explore the effects of new tobacco products (e.g., e-cigarettes) on the risk of lung cancer or conduct longitudinal tracking analyses in specific populations to enhance the breadth and depth of the study.
In conclusion, as a highly preventable disease, effective control of lung cancer incidence relies on interdisciplinary and cross-sectoral collaboration. This article emphasizes that global tobacco control strategies should be continuously promoted, especially in developing countries to increase intervention efforts, improve health literacy, and reduce the overall burden of tobacco-related diseases.
References
[1]. World Health Organization. (2021). Tobacco and cancer: Fact sheet. https: //www.who.int/news-room/fact-sheets/detail/tobacco
[2]. Smith, A., & Chen, L. (2018). Global smoking patterns and lung cancer mortality: A comparative study. Journal of Public Health, 22(4), 455–469.
[3]. Johnson, R. (2020). Tobacco use and disease burden: A review of longitudinal evidence. Epidemiology Review, 35(2), 89–103.
[4]. U.S. Department of Health and Human Services. (2014). The health consequences of smoking—50 years of progress: A report of the Surgeon General. Centers for Disease Control and Prevention. https: //www.cdc.gov/tobacco/data_statistics/sgr/50th-anniversary/
[5]. Our World in Data. (2023). Smoking and lung cancer statistics by country. https: //ourworldindata.org/smoking
[6]. Brown, T., et al. (2019). Lung cancer trends in the 21st century: A global perspective. International Journal of Cancer Research, 44(3), 245–260.
[7]. Marmot, M. (2015). The health gap: The challenge of an unequal world. Bloomsbury Publishing. https: //www.bloomsbury.com/us/health-gap-9781632860781/
[8]. GBD 2019 Risk Factors Collaborators. (2020). Global burden of 87 risk factors in 204 countries and territories, 1990–2019: A systematic analysis. The Lancet, 396(10258), 1223–1249. https: //www.thelancet.com/article/S0140-6736(20)30752-2/fulltext
[9]. World Health Organization. (2019). MPOWER: Measuring progress in tobacco control. https: //www.who.int/publications/i/item/9789241516204
[10]. Lee, H., et al. (2022). Economic evaluation of tobacco control policies. Journal of Health Economics, 59(2), 213–230.
Cite this article
Xiao,L. (2025). Global Public Health Perspective on the Impact of Cigarette Smoking on Lung Cancer Incidence. Theoretical and Natural Science,131,8-13.
Data availability
The datasets used and/or analyzed during the current study will be available from the authors upon reasonable request.
Disclaimer/Publisher's Note
The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of EWA Publishing and/or the editor(s). EWA Publishing and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content.
About volume
Volume title: Proceedings of ICBioMed 2025 Symposium: Interdisciplinary Frontiers in Pharmaceutical Sciences
© 2024 by the author(s). Licensee EWA Publishing, Oxford, UK. This article is an open access article distributed under the terms and
conditions of the Creative Commons Attribution (CC BY) license. Authors who
publish this series agree to the following terms:
1. Authors retain copyright and grant the series right of first publication with the work simultaneously licensed under a Creative Commons
Attribution License that allows others to share the work with an acknowledgment of the work's authorship and initial publication in this
series.
2. Authors are able to enter into separate, additional contractual arrangements for the non-exclusive distribution of the series's published
version of the work (e.g., post it to an institutional repository or publish it in a book), with an acknowledgment of its initial
publication in this series.
3. Authors are permitted and encouraged to post their work online (e.g., in institutional repositories or on their website) prior to and
during the submission process, as it can lead to productive exchanges, as well as earlier and greater citation of published work (See
Open access policy for details).
References
[1]. World Health Organization. (2021). Tobacco and cancer: Fact sheet. https: //www.who.int/news-room/fact-sheets/detail/tobacco
[2]. Smith, A., & Chen, L. (2018). Global smoking patterns and lung cancer mortality: A comparative study. Journal of Public Health, 22(4), 455–469.
[3]. Johnson, R. (2020). Tobacco use and disease burden: A review of longitudinal evidence. Epidemiology Review, 35(2), 89–103.
[4]. U.S. Department of Health and Human Services. (2014). The health consequences of smoking—50 years of progress: A report of the Surgeon General. Centers for Disease Control and Prevention. https: //www.cdc.gov/tobacco/data_statistics/sgr/50th-anniversary/
[5]. Our World in Data. (2023). Smoking and lung cancer statistics by country. https: //ourworldindata.org/smoking
[6]. Brown, T., et al. (2019). Lung cancer trends in the 21st century: A global perspective. International Journal of Cancer Research, 44(3), 245–260.
[7]. Marmot, M. (2015). The health gap: The challenge of an unequal world. Bloomsbury Publishing. https: //www.bloomsbury.com/us/health-gap-9781632860781/
[8]. GBD 2019 Risk Factors Collaborators. (2020). Global burden of 87 risk factors in 204 countries and territories, 1990–2019: A systematic analysis. The Lancet, 396(10258), 1223–1249. https: //www.thelancet.com/article/S0140-6736(20)30752-2/fulltext
[9]. World Health Organization. (2019). MPOWER: Measuring progress in tobacco control. https: //www.who.int/publications/i/item/9789241516204
[10]. Lee, H., et al. (2022). Economic evaluation of tobacco control policies. Journal of Health Economics, 59(2), 213–230.









